Blogs
Tympanometry in Otosclerosis: Role of Tympanometry in Diagnosing Conductive Hearing Loss
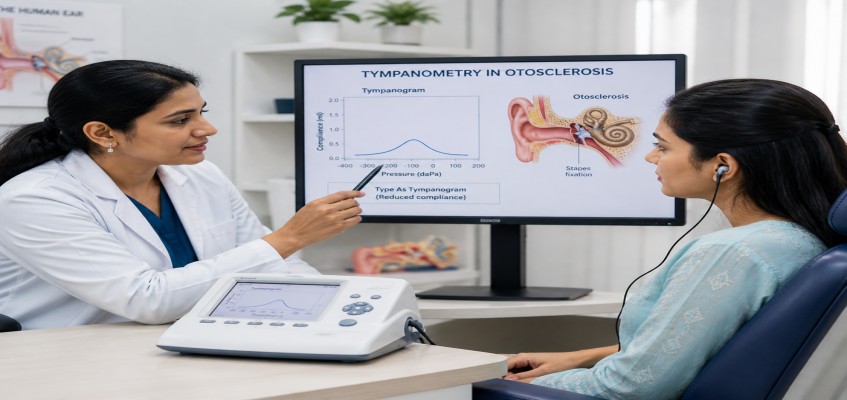
Tympanometry in otosclerosis is a quick test that checks how well your eardrum and middle ear move in response to gentle air pressure changes. It helps identify patterns that often appear when sound cannot pass efficiently through the middle ear.
In day to day ENT practice tympanometry in otosclerosis is most useful as a supportive test, not a stand alone answer. This article explains what tympanometry measures, what results are commonly seen in otosclerosis and how ENT specialists use it to narrow down the cause of conductive hearing loss. If you are evaluating treatment options, including surgery, understanding this test can help you have clearer conversations with your doctor.
How tympanometry helps in suspected otosclerosis
Otosclerosis is a condition where abnormal bone remodeling most often affects the stapes, a tiny middle ear bone. When the stapes become fixed, sound vibrations have difficulty reaching the inner ear. The result is typically conductive hearing loss, meaning sound transmission is reduced even when the inner ear may be healthy.
Because otosclerosis happens behind an eardrum that often looks normal, tests matter. Tympanometry in otosclerosis provides objective information about middle ear mobility and pressure, which helps an ENT team distinguish otosclerosis from other causes such as fluid, eardrum perforation or Eustachian tube problems.
Why conductive hearing loss needs careful testing
Conductive hearing loss has many possible causes. Some are temporary, such as middle ear fluid after a cold. Others are structural, such as ossicular chain problems or otosclerosis.
A key clinical challenge is that otosclerosis can present with gradually worsening hearing loss without pain, discharge or obvious infection signs. This is why tympanometry in otosclerosis is often ordered along with hearing tests to rule out more common, treatable middle ear conditions.
If you want a deeper overview of the condition itself, see Understanding Otosclerosis -Symptoms, Types, and Treatment Options.
What exactly does tympanometry measure
Tympanometry is a part of immittance testing. In simple terms it measures how the eardrum moves as air pressure changes in the ear canal. The test produces a graph called a tympanogram.
Your clinician will look at:
-
Peak pressure (whether middle ear pressure is normal or negative)
-
Compliance (how mobile the eardrum and middle ear system are)
-
Ear canal volume (helps interpret perforations or ventilation tubes)
In suspected conductive hearing loss, tympanometry helps identify whether the issue is likely related to stiffness, fluid, perforation or pressure dysfunction.
What does tympanometry in otosclerosis usually show
Tympanometry in otosclerosis often shows a pattern consistent with a stiffened system due to stapes fixation. The most classic finding is a Type As tympanogram, where the pressure peak is near normal but the height of the peak is reduced.
Is a “normal tympanogram” possible in otosclerosis
Yes. Tympanometry in otosclerosis can sometimes appear normal, especially in earlier stages or depending on equipment settings and individual anatomy. A normal tympanogram does not rule out otosclerosis.
This is why ENT specialists interpret tympanometry in otosclerosis alongside:
-
Pure tone audiometry results
-
Speech testing
-
Acoustic reflex testing
-
Clinical history and examination
What about acoustic reflexes
Many clinics pair tympanometry with acoustic reflex testing. In otosclerosis, stapes fixation often leads to absent acoustic reflexes, which can be a helpful clue.
So in practice tympanometry in otosclerosis is often less about one curve and more about the overall immittance profile.
Tympanometry patterns compared with other common causes
A major value of tympanometry in otosclerosis is differentiation. For example, fluid behind the eardrum commonly produces a flat tympanogram, while Eustachian tube dysfunction often shows negative pressure.
| Tympanogram pattern | Typical meaning | How it compares to otosclerosis |
|---|---|---|
| Type A (normal peak and height) | Normal middle ear pressure and mobility | Otosclerosis may still be present, especially early, so audiometry matters |
| Type As (shallow peak) | Stiffer system, reduced compliance | Common supportive finding in tympanometry in otosclerosis |
| Type B (flat) | Often middle ear effusion, sometimes perforation depending on ear canal volume | Less typical for otosclerosis, suggests fluid or perforation |
| Type C (negative pressure peak) | Often Eustachian tube dysfunction | Not typical for otosclerosis, may point to pressure-related issues |
This table highlights why tympanometry in otosclerosis is valuable: it helps rule in a stiffness pattern and rule out fluid or pressure problems that need different treatment.
Can tympanometry diagnose otosclerosis on its own
Tympanometry in otosclerosis supports diagnosis but usually cannot confirm it alone. Otosclerosis is ultimately a clinical diagnosis supported by audiology, reflexes and sometimes imaging.
Here is how ENT teams typically build diagnostic confidence.
Audiometry: the main test for hearing thresholds
Pure tone audiometry helps identify an air bone gap, which is a hallmark of conductive hearing loss. In many otosclerosis cases, audiometry may show patterns that suggest stapes fixation. Tympanometry in otosclerosis then adds evidence about middle ear mechanics.
Otoscopy: often normal, which is a clue
The eardrum often appears normal in otosclerosis. If the eardrum looks inflamed, retracted or perforated, the conductive loss may have a different cause and tympanometry will often reflect that.
Imaging: used selectively
High resolution CT of the temporal bone can be considered in selected cases. Imaging may help when the diagnosis is uncertain, symptoms are atypical or surgical planning requires more detail. Your ENT surgeon will decide whether it is needed.
What happens after tympanometry suggests otosclerosis
If the overall assessment points toward otosclerosis, your ENT specialist will discuss management based on hearing level, daily impact, ear status and patient preference.
Common options include:
-
Observation with periodic hearing tests
-
Hearing aids in suitable candidates
-
Surgery such as stapedectomy or stapedotomy when appropriate
For readers specifically exploring surgical care, you can learn more about finding a Best Stapedotomy surgeon in Kerala. If your case involves other middle ear reconstruction considerations, Ascent also provides advanced hearing restoration pathways through its cochlear and middle ear expertise, including information relevant to patients searching for the Best ossiculoplasty surgeon in kerala and the Best Cochlear implant specialist in kerala.
It is also important not to confuse terms that sound similar. Tympanosclerosis is a different condition involving scarring or calcification of the eardrum or middle ear tissues. If you have been told that diagnosis, see Tympanosclerosis Treatment: Medical & Surgical Options.
When should you see an ENT specialist
Consider an ENT evaluation if you have:
-
Gradually worsening hearing in one ear or both ears
-
Difficulty hearing in meetings or family conversations
-
A sense that hearing is muffled without pain or fever
-
A family history of otosclerosis
Early evaluation matters because tympanometry in otosclerosis works best when combined with complete assessment and timely follow up.
If you are looking for an experienced ENT clinic in Kerala with comprehensive diagnostics and surgical expertise, Ascent ENT Hospital Kerala offers full ear nose and throat services including advanced hearing assessment.
Why patients choose Ascent for hearing loss evaluation
Ascent Hospital is widely recognized as the best ENT Hospital in Kerala for many patients seeking specialty care, with dedicated ENT services and modern diagnostic facilities. The clinical team uses structured evaluation pathways where tympanometry in otosclerosis is interpreted alongside audiometry and specialist examination to reach the right diagnosis and recommend the safest next step.
You can explore the hospital and services through Ascent Hospital.
Conclusion
Tympanometry in otosclerosis is an important supportive test that helps ENT specialists evaluate middle ear stiffness and narrow down causes of conductive hearing loss. A Type As tympanogram and absent acoustic reflexes can strengthen suspicion, while normal results do not fully rule it out. The most accurate diagnosis comes from combining tympanometry, audiometry, clinical examination and selected imaging.
If you have concerns about hearing loss or you have been advised to undergo tympanometry in otosclerosis, the next best step is a specialist consultation. Schedule an appointment with the team at Ascent, the best ENT Hospital in Kerala, via the contact page to plan a complete hearing evaluation and discuss the right treatment options for you.
Share
Share on WhatsAppOur Professionals
Our Patient Stories
View All Testimonials






.jpeg)






































